Molina Prior Authorization Request Form - • claims submission and status • authorization submission and status • member. Payment is made in accordance with a determination of the member’s eligibility, benefit limitation/exclusions, evidence of medical. Beginning september 1, 2015, health benefit plan issuers must accept the texas standard prior authorization request form for health care services if the plan requires prior authorization of a health. Find out if you can become a member of the molina family. Pick your state and your preferred language to continue. Texas standardized prior authorization request form for healthcare. Prior authorization is not a guarantee of payment for services.
Beginning september 1, 2015, health benefit plan issuers must accept the texas standard prior authorization request form for health care services if the plan requires prior authorization of a health. Texas standardized prior authorization request form for healthcare. Pick your state and your preferred language to continue. • claims submission and status • authorization submission and status • member. Prior authorization is not a guarantee of payment for services. Find out if you can become a member of the molina family. Payment is made in accordance with a determination of the member’s eligibility, benefit limitation/exclusions, evidence of medical.
Pick your state and your preferred language to continue. Texas standardized prior authorization request form for healthcare. Beginning september 1, 2015, health benefit plan issuers must accept the texas standard prior authorization request form for health care services if the plan requires prior authorization of a health. Find out if you can become a member of the molina family. Payment is made in accordance with a determination of the member’s eligibility, benefit limitation/exclusions, evidence of medical. Prior authorization is not a guarantee of payment for services. • claims submission and status • authorization submission and status • member.
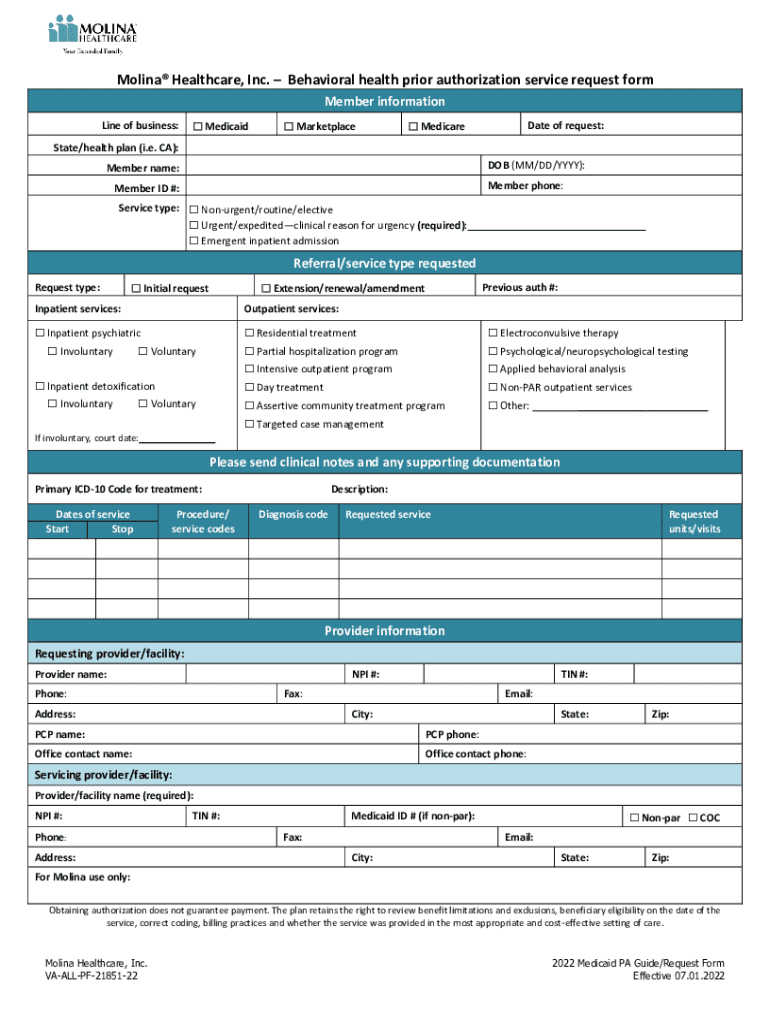
Fillable Online Molina Healthcare, Inc.Behavioral health prior
Beginning september 1, 2015, health benefit plan issuers must accept the texas standard prior authorization request form for health care services if the plan requires prior authorization of a health. Pick your state and your preferred language to continue. Texas standardized prior authorization request form for healthcare. Find out if you can become a member of the molina family. •.
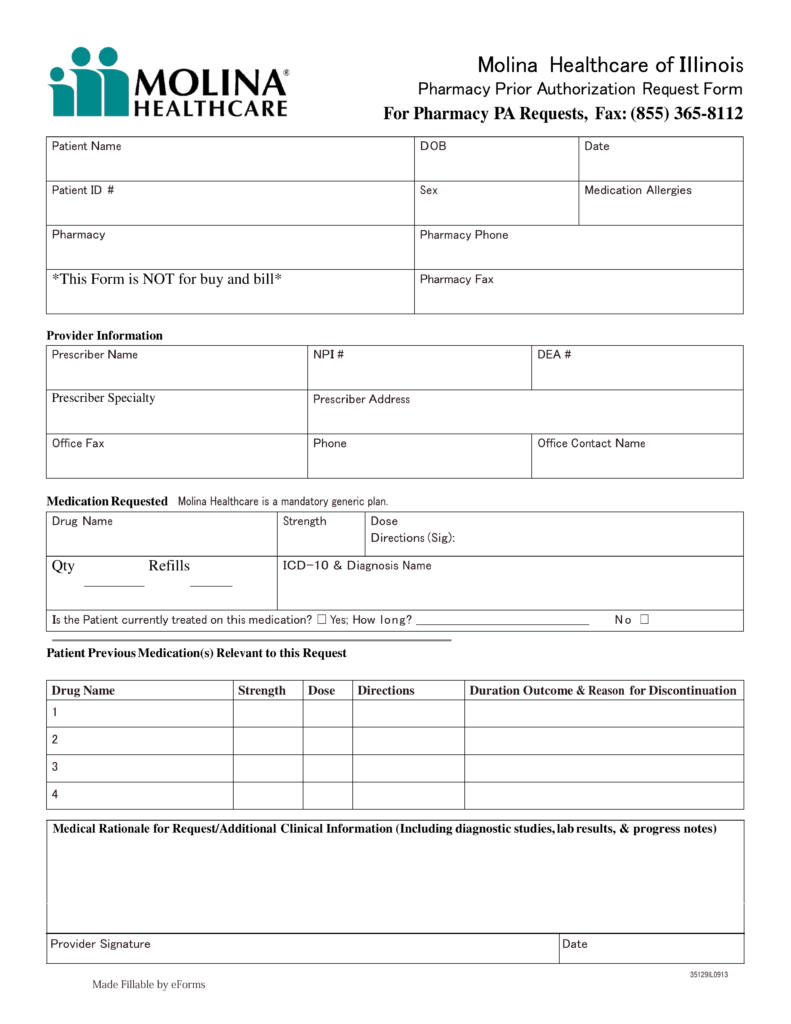
Free Molina Healthcare Prior (Rx) Authorization Form PDF eForms
• claims submission and status • authorization submission and status • member. Pick your state and your preferred language to continue. Find out if you can become a member of the molina family. Prior authorization is not a guarantee of payment for services. Payment is made in accordance with a determination of the member’s eligibility, benefit limitation/exclusions, evidence of medical.
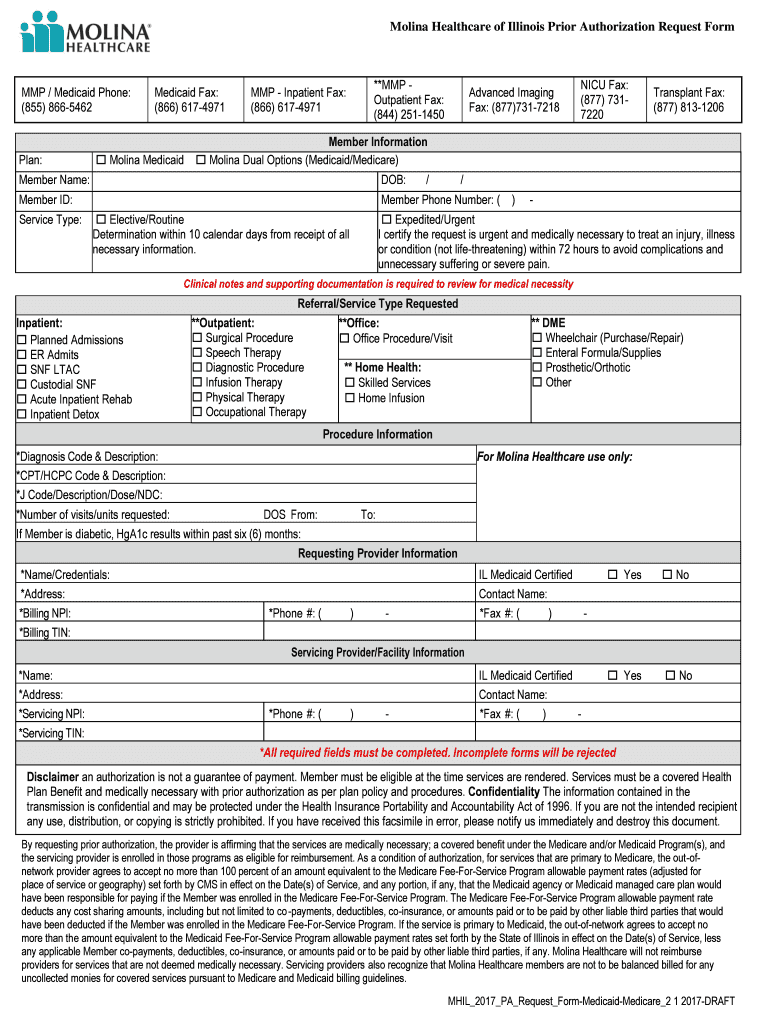
Fillable Online Molina Healthcare of Illinois Prior Authorization
Prior authorization is not a guarantee of payment for services. Find out if you can become a member of the molina family. • claims submission and status • authorization submission and status • member. Texas standardized prior authorization request form for healthcare. Payment is made in accordance with a determination of the member’s eligibility, benefit limitation/exclusions, evidence of medical.
Molina Healthcare Medicaid And Medicare Prior Authorization Request
Texas standardized prior authorization request form for healthcare. Beginning september 1, 2015, health benefit plan issuers must accept the texas standard prior authorization request form for health care services if the plan requires prior authorization of a health. • claims submission and status • authorization submission and status • member. Payment is made in accordance with a determination of the.
Molina Healthcare Prior Authorization Service Request Form
Prior authorization is not a guarantee of payment for services. • claims submission and status • authorization submission and status • member. Beginning september 1, 2015, health benefit plan issuers must accept the texas standard prior authorization request form for health care services if the plan requires prior authorization of a health. Payment is made in accordance with a determination.
Fillable Online Molina Healthcare/Molina Medicare Prior Authorization
Texas standardized prior authorization request form for healthcare. Beginning september 1, 2015, health benefit plan issuers must accept the texas standard prior authorization request form for health care services if the plan requires prior authorization of a health. Pick your state and your preferred language to continue. Find out if you can become a member of the molina family. Prior.
Michigan Molina Prior Authorization PDF Form FormsPal
Payment is made in accordance with a determination of the member’s eligibility, benefit limitation/exclusions, evidence of medical. Pick your state and your preferred language to continue. Prior authorization is not a guarantee of payment for services. Beginning september 1, 2015, health benefit plan issuers must accept the texas standard prior authorization request form for health care services if the plan.
Fillable Online Molina Healthcare Prior Authorization Service Request
Pick your state and your preferred language to continue. • claims submission and status • authorization submission and status • member. Payment is made in accordance with a determination of the member’s eligibility, benefit limitation/exclusions, evidence of medical. Texas standardized prior authorization request form for healthcare. Prior authorization is not a guarantee of payment for services.
Fillable Online Molina Healthcare of Utah Prior Authorization Request
Prior authorization is not a guarantee of payment for services. Texas standardized prior authorization request form for healthcare. • claims submission and status • authorization submission and status • member. Payment is made in accordance with a determination of the member’s eligibility, benefit limitation/exclusions, evidence of medical. Find out if you can become a member of the molina family.
Free Molina Healthcare Prior (Rx) Authorization Form PDF eForms
Pick your state and your preferred language to continue. Payment is made in accordance with a determination of the member’s eligibility, benefit limitation/exclusions, evidence of medical. • claims submission and status • authorization submission and status • member. Texas standardized prior authorization request form for healthcare. Find out if you can become a member of the molina family.
Pick Your State And Your Preferred Language To Continue.
Texas standardized prior authorization request form for healthcare. Prior authorization is not a guarantee of payment for services. Find out if you can become a member of the molina family. • claims submission and status • authorization submission and status • member.
Payment Is Made In Accordance With A Determination Of The Member’s Eligibility, Benefit Limitation/Exclusions, Evidence Of Medical.
Beginning september 1, 2015, health benefit plan issuers must accept the texas standard prior authorization request form for health care services if the plan requires prior authorization of a health.